Human 3D cell-based systems to research gout: drug discovery for a neglected disease
Posted: 18 December 2020 | Hannah Balfour (Drug Target Review) | No comments yet
In this article Andrew Nyborg from Horizon Therapeutics discusses why researchers are taking a second look at gout and how they are modelling the condition, which is unique to humans.


“Gout is a neglected disease. While there is a drug to treat the underlying cause, it was discovered more than 50 years ago and very little innovation has occurred since then, as most new drugs entering clinical trials have a very similar mechanism of action,” explained Andrew Nyborg, Senior Director of Development Sciences at Horizon Therapeutics. Nyborg and his team at Horizon, in partnership with HemoShear Therapeutics, a clinical stage company developing treatments for metabolic disorders, have been working to identify novel drug targets for gout and are currently synthesising and validating molecules to target them.
“This would be fine if these drugs were effective in all gout patients, but some who receive these drugs can still experience excruciating pain. This is debilitating and makes their lives extremely difficult. What is interesting is that gout is not rare – with some 9.2 million patients suffering from it in the US – nor is it a tropical disease, as so many other neglected diseases are. For the cohort with severe gout, there is clear unmet medical need and therefore we want to explore whether there may be more effective targets and the potential to develop new treatments with novel mechanisms of action.”
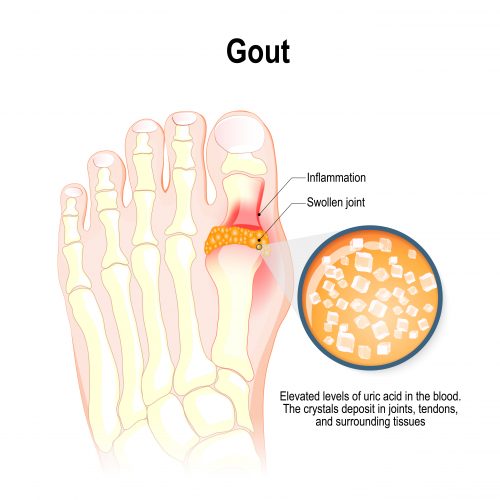
Gout is the development of arthritis due to the deposition of monosodium urate crystals in the joints and connective tissue. It is the most common form of inflammatory arthritis and particularly common in the smaller bones of the feet. Uric acid, a waste by-product of purine metabolism, circulates in the blood as urate ions. Once a state known as hyperuricemia (over-saturation of the blood serum with urate [at urate levels of over 6.8mg/dL]) is reached, urate interacts with sodium ions and water to form insoluble monosodium urate crystals that accumulate in the joints. These crystals activate tissue-resident macrophages and the complement system, causing a release of pro-inflammatory cytokines such as IL-1β and an influx of neutrophils, which then proceed to secrete further pro-inflammatory factors.1 The result is joint inflammation, pain and tissue damage.

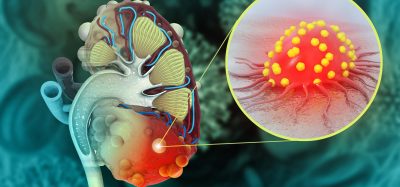
If uric acid levels are left unmanaged, these crystals can also deposit in certain organs. They are most often found in highly vascularised organs (eg, the kidneys, heart and lungs), given that uric acid is circulated in the blood. The long-term consequences of these uric acid deposits in organs are currently an active area of research, said Nyborg.
He explained that studying gout and identifying targets for drug development has been limited by the available models: “Elevated uric acid is unique to humans and a handful of other higher primates because every other animal on Earth expresses an enzyme called uricase. Uricase oxidises uric acid to a much more soluble product called allantoin. As we lack this enzyme, humans tend to have elevated uric acid and are therefore prone to gout.”
Modelling for distinctly human diseases
There are many types of three-dimensional (3D) human cell-based systems, including organoids, organs-on-a-chip and hemodynamic flow systems.
Derived from human tissue, they are an essential tool for modelling complex human diseases – including gout – outside the body but in a system where the signalling patterns, pathophysiology and disease states are conserved, Nyborg commented.
…scientists are hopeful that they can develop therapies with novel mechanisms of action that can meet some of the unmet medical need in patients”
“Gout is just one example of why these human 3D cell-based model systems are important. For many years, scientists have been attempting to use rodent models to study the condition, but because they express the uricase enzyme their fundamental biology prevents them from being an accurate model,” said Nyborg.
Some important uses of human cell-based systems, eg, organoids, include the study of age-related disorders like neurodegeneration, where the life-span of animals is insufficient to replicate the course of the human disease; the development of personalised medicine; and studies of infectious diseases, such as respiratory syncytial virus, hepatitis B and COVID-19. For some of these applications, it is preferable to derive the organoids from tissue samples taken from donors with the disease. However, Nyborg explained that for their model this was not necessary: “We have discovered that whether cells come from healthy patients or those with gout, they signal in pretty similar fashions once we introduce elevated levels of uric acid. From our research, it appears there is a pretty fine line between being a non-gout or a gout patient, with only a small increase in uric acid levels maintained over a long period of time being sufficient to cause the devastating phenotype associated with gout”.
Modelling gout
Horizon is currently collaborating with HemoShear to discover more about gout. In the partnership, researchers deploy a hemodynamic 3D liver cell system exposed to high levels of uric acid and monosodium urate crystals, to develop the gout phenotype and then perform transcriptomic analysis. The data from these analyses are then used to create an in silico model system with HemoShear’s proprietary platform, REVEAL-Tx™.

Using the computer simulations, researchers can investigate which pathways are involved in gout. Nyborg said this is particularly exciting, as it allows them to explore the possibility of novel targets that could allow for the development of new, more beneficial therapies for patients. He added that in the past they did not have the capabilities to probe such questions, which prevented progress in identifying or generating novel gout therapies.
According to Nyborg, over the past year and a half, the team has identified several novel targets and validated them in model systems. The team is also developing functional assays, which they believe can accurately reproduce the gout disease state and therefore be used for the screening of the potential drug candidates.
“Typically, when we say pre-clinical testing, people tend to envision animal models. At this stage, we are really looking at how well we understand gout and establishing the efficacy of candidates in a human system.”
Conclusion
Using a combination of human 3D cell-based systems and computer simulations, the researchers aimed to gain a better understanding of gout and the pathways implicated in the disease. The scientists are hopeful that they can develop therapies with novel mechanisms of action that can meet some of the unmet medical need in patients with the severest form of the condition.
Nyborg highlighted the importance of using human-based modelling systems when researching diseases such as gout – which are either unique to humans or where the basic biology of animal models cannot accurately recreate the condition. He concluded that he is excited about taking a new approach to tackle a disease that people believed was well understood and was therefore not worthy of further exploration or improved treatment options.
Reference
- Martillo MA, Nazzal L, Crittenden DB. The crystallization of monosodium urate. Curr Rheumatol Rep. 2014;16(2):400. doi: 1007/s11926-013-0400-9
Related topics
Cell Cultures, Cell-based assays, Disease Research, Drug Development, Drug Targets, In Vitro, Lead Generation, Organoids, Research & Development, Small Molecules, Therapeutics
Related conditions
Covid-19, Gout, Hepatitis B, neurodegeneration, respiratory syncytial virus (RSV)
Related organisations
HemoShear Therapeutics, Horizon Therapeutics
Related people
Andrew Nyborg (Horizon Therapeutics)